Imagine dealing with painful mouth and/or genital ulcers, eye pain or skin rashes that keep returning without any explanation. For people with Behcet’s disease, this is often a reality. Also called Behcet’s syndrome, it is a rare, chronic autoinflammatory disorder where the immune system attacks the body’s blood vessels. The condition can affect many organs, including the mouth, eyes, skin, joints, gut and nervous system. Let’s find out all that there is to know about this syndrome.
What is Behcet’s disease?
Behcet’s is classified as an autoinflammatory vasculitis, meaning it causes inflammation in blood vessels of all sizes. Unlike many autoimmune diseases, it tends to flare up unpredictably, with symptom-free time periods followed by relapses. Because it can affect multiple systems, the disease looks different in every patient, making it difficult to diagnose early.
Symptoms of Behcet’s disease
As we have already discussed, symptoms for Behcet’s disease may vary, but the most common include:
- Oral ulcers: Painful sores in the mouth that heal and return frequently.
- Genital ulcers: Painful lesions in both men and women.
- Skin problems: Acne-like rashes, red nodules (erythema nodosum), or inflammation in veins (thrombophlebitis).
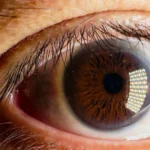
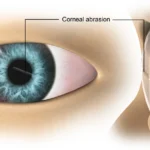
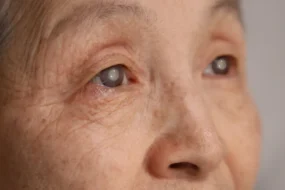
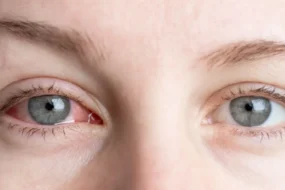
- Eye inflammation (uveitis): Redness, blurred vision, eye pain and floaters. If untreated, this can cause permanent vision loss.
- Joint pain: Arthritis-like swelling, especially in knees, ankles and wrists.
- Digestive issues: Abdominal pain, diarrhoea (sometimes bloody) and nausea.
- Vascular involvement: Deep vein thrombosis, aneurysms or cerebral venous thrombosis in severe cases.
- Neurological symptoms: Headaches, memory problems, paralysis or seizures, caused by inflammation in the brain or spinal cord.
- Some patients also show a pathergy reaction, where a small needle prick leads to exaggerated skin swelling or redness.
Causes and risk factors
Behcet’s disease is not contagious. Although the exact cause is still unknown, several factors could be responsible for Behcet’s disease such as:
- Genetics: People carrying the HLA-B51 gene have a higher risk.
- Geography and ethnicity: More common in Asia and the Mediterranean.
- Age and gender: Typically diagnosed between ages 20 to 40 years; men often have more severe cases of the disease.
- Environment: Infections or unknown environmental triggers may influence flares.
How is Behcet’s disease diagnosed?
There is no single test to diagnose the Behcet’s syndrome. Doctors rely on a combination of medical history, physical examination and exclusion of other conditions. Diagnosis is often based on:
- At least three oral ulcer episodes in a year, plus two of the following – genital ulcers, skin lesions, eye inflammation or a positive pathergy test.
- Blood tests, imaging (X-ray, CT, MRI) or skin biopsy to rule out other causes.
- Ophthalmology exams to check for eye inflammation.
Treatment options for Behcet’s disease
There is currently no cure, but treatment can help control inflammation and reduce flare-ups. Treatment options for the Behcet’s disease include:
1. Corticosteroids
For mild symptoms, topical creams, mouth rinses or drops are useful. However, for severe inflammation, oral or injected steroids can be helpful. Long-term use carries side effects like weight gain, osteoporosis and high blood pressure.
2. Immunosuppressants
Medicines such as azathioprine, ciclosporin, colchicine and tacrolimus calm the immune system and help prevent relapses. In severe cases, developing the first therapeutic antibody ‘alemtuzumab’ may be of benefit.
3. Biologic therapies
TNF-alpha inhibitors like infliximab or adalimumab are prescribed for severe or resistant disease.
4. Pain relief
Non-steroidal anti-inflammatory drugs (NSAIDs) for joint and muscle pain.
5. Symptom-specific care
Migraine treatments for headaches, special drops for eye inflammation, or surgery in rare cases of GI bleeding or aneurysms.
6. Pregnancy considerations
Fertility is usually not affected, but some medicines (like thalidomide, methotrexate and cyclophosphamide) can harm the unborn baby. Patients planning a family should consult their doctor to adjust the treatment safely.
Living with Behcet’s disease
Alastair Lockwood at Feel Good Contacts shares that “Managing Behcet’s requires consistent care and lifestyle adjustments. Besides monitoring flare-ups and possible triggers such as stress or infections, patients at risk should also adopt healthy habits like balanced nutrition, gentle exercise and quality sleep. Additionally, they should seek support of patient groups and talk to counsellors to manage the emotional impact. If possible, they should also inform their teachers or employers to help accommodate flare periods.”
In the UK, patients may be referred to one of three NHS Behcet’s Centres of Excellence (London, Birmingham and Liverpool), which provide specialist multi-disciplinary care.
FAQs
Is Behcet’s disease life-threatening?
Most people live well with treatment, but complications involving major organs can be serious without special care.
Can Behcet’s disease be cured?
No specific cure exists for this syndrome, but treatment significantly reduces symptoms.
What triggers flare-ups in Behcet’s disease?
Stress, infections and sometimes environmental factors can play a crucial role in triggering flare-ups.
Is Behcet’s disease hereditary?
Having certain genes increases the risk but does not guarantee inheritance. The chances of passing Behcet’s disease on hereditarily are very bleak.
Which doctor should I consult for Behcet’s disease?
Usually, you’ll need a mix of specialists to live with the syndrome. You can consider a rheumatologist, supported by dermatologists, ophthalmologists, neurologists and oral medicine experts.