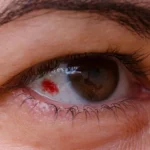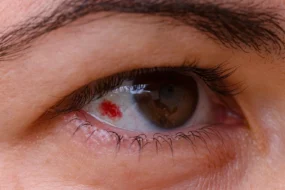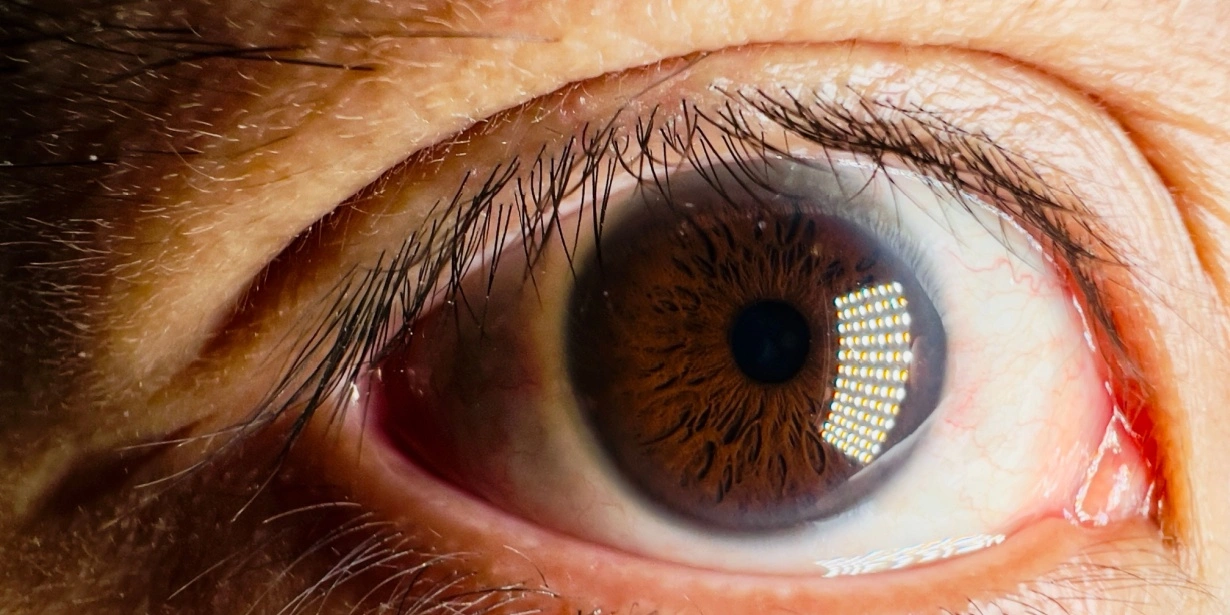
Diabetic retinopathy is a complication of diabetes that affects the eyes. It happens when high blood sugar levels damage the tiny blood vessels in the retina, the light-sensitive layer at the back of the eye. If it is not detected and managed early, it can lead to serious vision problems and even blindness.
Research shows that almost 5 million people in the UK live with diabetes and a significant number develop some level of Diabetic Retinopathy over time. Read on to know what causes diabetic retinopathy, symptoms, stages, treatment options and more.
How Does Diabetes Affect the Retina?
The retina plays a key role in helping you see clearly by sending signals through the optic nerve to the brain. When blood sugar levels remain high, they start damaging the small blood vessels in the retina, causing them to:
- Swell
- Leak fluid or blood
- Become blocked
In more advanced stages, unmanaged diabetes may lead to the growth of new abnormal blood vessels. These vessels can bleed easily, leading to further complications.
Diabetic Retinopathy Symptoms
In the early stages, it may be harder to spot noticeable signs, which is why getting regular eye exams is essential. However, as the condition progresses, common symptoms of diabetic retinopathy include:
- Blurred or distorted vision
- Floaters or dark spots
- Difficulty seeing at night
- Sudden changes in vision
Diabetic Retinopathy Stages
It develops in three stages, usually getting worse gradually, over the course of several years. These stages are:
1. Background retinopathy
This is the earliest stage, also known as stage 1 diabetic retinopathy. In this stage, tiny bulges develop in the blood vessels of the retina and may leak small amounts of blood. Your vision is usually not affected in this stage, so there’s hardly any need of treatment. However, the risk of developing problems may arise later, highlighting the need of regular monitoring.
2. Pre-proliferative retinopathy
At this stage, the damage becomes more visible with some blood vessels getting blocked and retina’s blood flow getting affected. While vision may still not be noticeably affected, vision problems are expected to follow. More frequent eye screening is usually recommended to monitor any changes closely.
3. Proliferative retinopathy
This is the most advanced stage of diabetic retinopathy, wherein new, fragile blood vessels grow on the retina and can bleed into the eye. At this point, there is a high risk of sight loss. Specialist treatment is required to help protect and preserve vision.
4. Diabetic maculopathy
Diabetic maculopathy isn’t a stage but a related condition that can develop during any of the above-mentioned stages. It affects the macula, the central part of the retina, making it difficult to read clearly. However, your peripheral (side) vision may be fine.
Treatment Options
In most cases, the damage caused by diabetic retinopathy is irreversible. However, if it is detected early, treatment and good diabetes control can stop it from getting worse. Treatment depends on the severity of the condition. As mentioned above, you may not need treatment straight away but only regular monitoring in the initial stages. For more advanced stages, treatment options include:
- Anti-VEGF treatment
Anti-VEGF medication is given as an eye injection using a tiny needle. It works by blocking a protein that, when present in high levels, causes blood vessels to leak and abnormal new vessels to grow. This treatment also helps reduce retinal swelling and protect vision.
- Laser treatment
This treatment uses a laser to seal leaking blood vessels in the retina, helping prevent further leakage and slow the growth of abnormal blood vessels. The laser creates small, controlled burns in the affected areas to stabilise the condition and protect vision.
- Steroid implants
These implants are placed inside the eye just like an injection. They slowly release medication over time to reduce swelling and inflammation. They are often used to treat long-term fluid build-up in the macula.
- Surgery
Eye surgery may be needed in advanced cases to remove blood or scar tissue from the back of the eye, helping stabilise the condition and protect remainingvision.
How to Prevent Diabetic Retinopathy from Worsening?
While diabetic retinopathy cannot always be prevented, here are simple steps you can take to reduce the risk of it progressing:
- Keep blood sugar levels within your target range
- Manage blood pressure and cholesterol
- Attend regular diabetic eye screening appointments
- Follow a healthy, balanced diet
- Stay physically active
- Avoid smoking and limit alcohol intake
Diabetic retinopathy is a serious eye condition. However, with early detection, regular eye check-ups and blood sugar control, its progression can often be slowed. Staying proactive about your eye health can help protect your vision over time.
Disclaimer: The advice in this article is for informational purposes only and does not replace medical care or an in-person check-up. Please check with an eyecare professional before purchasing any products or remedies. For information on our article review process, please refer to our Editorial Policy.